Evaluation of Acute Wounds in the Hand and Upper Extremity
- PGH ORTHO
- Aug 30, 2020
- 4 min read
Nathaniel S Orillaza Jr.
Associate Professor
Department of Orthopedics
University of the Philippines - Manila College of Medicine
Orthopedics deals with all types of acute wounds in the emergency room. Appropriate evaluation and initial care at the emergency room contribute to prevention of complications and planning for definitive management.
Classification of Wounds
There are different published classifications of wounds available. A more practical approach, proposed in the Lister’s Hand Diagnosis and Indications (Smith, 2001), uses easy to understand descriptions to categorize wounds in the hand and upper limb.
Tidy wounds are those inflicted by sharp instruments and have well-defined edges. They may present as lacerations, sliced with or without skin flaps or puncture wounds. These wounds tend to heal primarily with minimal scarring.


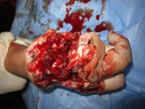
Untidy wounds result from tearing or bursting of the skin caused by crushing, explosions and heavy equipment (e.g. rollers, power-saws, industrial and farm machineries). The edges may have irregular flaps with doubtful viability and might require more complex procedures for coverage.
Fingertip injuries and amputations are described separately.
Evaluation at the Emergency Room
At the ER, during resuscitation, do not forget that it is possible for patients to become unstable or even die if bleeding is not monitored, especially for those who had some delays during transport. Vital signs are still important and will need to be part of the holistic management. Even if things are literally falling apart, it is important to take a good history especially the mechanism and the time of injury. It helps to ask specifics on the injuring device and the position and reaction of the patient during the injury. Sudden retractions from machines result to avulsion of tissues.
Occasionally, the mechanism of injury is obvious but remember to resist the urge to just pull out penetrating and other attached materials as it may result to more damage.
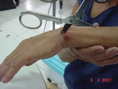
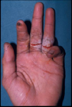
When examining wounds, knowledge of anatomy helps anticipate structures that are also involved underneath. This helps streamline the evaluation to limit discomfort to patients. Notice findings that may point to specific tissues like unusual hand postures and lack of tenodesis effect pointing to a possible tendon injury or obvious sensory deficit pointing to specific nerve transections. The figure on the left below shows extension of the middle and ring fingers with wounds over the flexor tendons, pointing to FDP and FDS transection. The location of the wound at the base of the thumb on the right, hints to a possible involvement of the digital nerves.
Control of Wound Bleeding
When encountering profuse bleeding on inspection, it is important to NEVER blindly clamp vessels. This tends to do more harm than good. Tourniquets, while useful in some situations, is largely discouraged in a hospital setting. This brings an additional risk of being left unmonitored and causing ischemia.
The simplest and often effective way of controlling bleeding in the upper limb involves elevation, compressive bandaging and applying pressure on the proximal vessels like the brachial artery.

Initial management
The initial step in managing patients with open wounds include copious irrigation to wash off contaminants and microorganisms. Clean tap water is enough for the purpose, based on current recommendations. Simultaneously, tetanus prophylaxis is initiated or updated. Antibiotics are added for the untidy and deeper wounds, adjusting coverage to the type and degree of contamination.
Several layers of absorbent materials, like gauze, held in place by elastic bandage, is preferred to protect from contamination. While it is usual to apply a circular bandage for most parts of the limb, avoid doing this in the fingers as it may lead to distal necrosis. Instead, use fluffy, breathable dressing with enough layers to absorb blood and exudates, and make sure that the inter-digital areas are dressed to avoid maceration.

Amputations
One important injury that causes panic and anxiety to many medical students in the emergency room, around the world, is amputations. These injuries, in practice, are relative emergencies and are better managed with proper preservation of the severed part and preparation of the patient and surgical team. In the initial encounter, ensure that the detached part is placed in a moist (wrapped in gauze wet with Ringer’s or Saline solution), sealed container, preserved in a cool (not frozen) environment like an ice bucket. A properly preserved part without muscle (distal to intrinsic muscles) may last for 12 hours in war ischemia or up to 24 hours in cold ischemia. The presence of muscles in more proximal aputations, cuts the estimates in half.

Image Source: American Society for Surgery of the Hand
To prepare the patient for surgery, ensure adequate fasting time for anesthesia, while supporting with intra-venous hydration. Inform the specialty team ahead of transfer or upon arrival to give adequate time for preparation.
Fingertip injuries
Fingertip injuries are common in children and the working age group and vary in presentation. Like most open wounds, the priority is to irrigate the wound and remove as much contamination. Evaluation includes identification of depth and exposure of tissues that may not heal without additional coverage like bones and tendons. For wounds without coverage issues, maintaining a moist, non-infected environment are adequate to allow timely secondary healing. Nailbed lacerations, when present, should be properly repaired to avoid symptomatic nail deformities.
Special Considerations
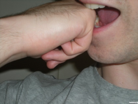
Some wounds warrant urgent attention as they are known to be related to devastating complications. Wounds connected to fractures (still considered open fractures even in small bones) require antibiotic prophylaxis and debridement. Wounds in certain locations like the knuckles, with or without the patient admitting being in a fist fight, should be considered as a possible human bite, unless proven otherwise. Neglect may lead to deep and progressive infection. Small penetrating wounds through muscle compartments may seem innocuous but bleeding in a tight compartment may lead to compartment syndrome.
Complications
Inadequate evaluation and care for acute wounds in the emergency setting may lead to the complications like infection that may become chronic, spread locally and result to more tissue loss, or systemically which may cost the patient’s life.